 Leading last year's Atlanta Walk to End Lupus Now
Leading last year's Atlanta Walk to End Lupus Now As many of you know my team, the Lupus Racing Team, is in a really unique and cool position within the ranks of Continental Pro Cycling teams in that we aren’t just racing to win and bring recognition to the brands that sponsor us, but also, to raise awareness to a mysterious disease that affects about 5 million people in the world with no known cure. The team began when our general manager’s wife asked a simple question, “Why don’t cycling team’s ever benefit the greater good?” Sparked by this idea and his ambition to run a cycling team the Lupus Racing Team was born in 2012. Brendan's and Stephen Jamison's (the team's owner) dream continued as the team received a professional license in 2015 and continues to build on it’s success on the road while reaching people about the mystery of Lupus this year.
This week is especially important as the Lupus Foundation of America’s (LFA) Georgia Chapter puts on the Atlanta Walk to End Lupus Now this Saturday, April 30th. It is the largest fundraising walk for any U.S. Chapter of LFA. Our team’s base in Atlanta makes this an important part of our goal to raise awareness of the lack of a cure for Lupus and help raise money for further research. Many reading may not know exactly what Lupus is and I want to use this blog as an opportunity to fill you in on what Lupus is and where the research stands. I also want to share with you a couple personal stories/interviews from Marjorie Sullivan and Melissa Higginson, both sufferers of Lupus involved with the team. Marjorie’s discussion with the team at Camp really opened my eyes to the mystery and cruelness of the disease that isn’t represented from a quick Google search. I hope these stories will have a similar effect for you. If you feel the urge to give, however small the gift, our team, and the Lupus community would be very grateful. Press the button below to donate as part of the Lupus Racing Team group. If not led to give I urge you to read through this piece and help us in our goal to raise awareness for the disease. Thanks!
This week is especially important as the Lupus Foundation of America’s (LFA) Georgia Chapter puts on the Atlanta Walk to End Lupus Now this Saturday, April 30th. It is the largest fundraising walk for any U.S. Chapter of LFA. Our team’s base in Atlanta makes this an important part of our goal to raise awareness of the lack of a cure for Lupus and help raise money for further research. Many reading may not know exactly what Lupus is and I want to use this blog as an opportunity to fill you in on what Lupus is and where the research stands. I also want to share with you a couple personal stories/interviews from Marjorie Sullivan and Melissa Higginson, both sufferers of Lupus involved with the team. Marjorie’s discussion with the team at Camp really opened my eyes to the mystery and cruelness of the disease that isn’t represented from a quick Google search. I hope these stories will have a similar effect for you. If you feel the urge to give, however small the gift, our team, and the Lupus community would be very grateful. Press the button below to donate as part of the Lupus Racing Team group. If not led to give I urge you to read through this piece and help us in our goal to raise awareness for the disease. Thanks!
 Marjorie (Left) and Melissa
Marjorie (Left) and Melissa Before we get started let me introduce Marjorie Sullivan and Melissa Higginson. Marjorie is Brendan's (our GM) wife and the lady who really jump started this team to be a voice of awareness for Lupus. She is involved within the Lupus community in Georgia and her story at camp really opened my eyes to the difficulties this disease presents. Melissa is the house mom for the team at the Redlands Bicycle Classic and thrives in the role. She is an awesome host and a wonderful connection between the cycling community and the Lupus community. In Theory both Marjorie and Melissa have mild or "good" Lupus, but after you hear part of their story I'm sure you'll agree with me that there isn't a "good" Lupus. I asked them both a couple general questions and have molded their responses into the "story" below, but provided full transcripts to their responses at the bottom of the blog for more in depth look at the disease, the struggles, and life with Lupus from their point of view.
What is Lupus?
 Logo Representing unknowns of Lupus
Logo Representing unknowns of Lupus Little is known about Lupus, but it is a chronic (meaning lasting longer than 6-weeks), autoimmune disease, meaning your body (immune system) attacks healthy tissues (cells) because it believes they are foreign invaders [1]. Lupus doesn’t attack one specific area of the body but may affect many different systems, such as your joints, skin, blood cells, brain, heart and lungs [2]. The many areas affected causing a multitude of symptoms make it extremely complicated to determine if a person has Lupus. Furthermore, the disease flares and remises meaning symptoms are often gone unchecked as they come and go [1]. It is estimated that 5 million people in the world (1.5 Million in the U.S.) have Lupus. While anyone can suffer from Lupus it is much more prolific in women of childbearing age (15-44) and 2-3x more likely in women of color [1]. Approximately 9 out of 10 people with Lupus are women[3]. Lupus can come in many forms from mild to life-threatening, and while there is still no cure, current medical technology means most people with Lupus will not die from the disease [1].
Causes, Diagnosis, and Symptoms
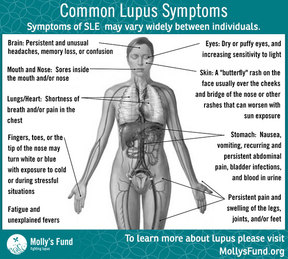
The direct cause for Lupus is unknown, but researches believe it is a combination of genetics and one’s environment. Although no gene has been linked directly to Lupus it does seem to appear in certain families and if one of two identical twins have it, the other is more likely to develop the disease[6]. Potential triggers for the disease include sunlight, infections, or medications[2]. The symptoms of Lupus are often hard to detect due to the remissive behavior along with it’s variability among patients. Lupus is sometimes described as “The Great Imitator” as it’s symptoms mimic a multitude of other diseases. The one distinct symptom synonymous with Lupus is the butterfly rash that can appear between the cheeks on someone’s face. When diagnosing a patient a doctor will look for a combination of the following symptoms.
- Extreme fatigue (tiredness)
- Headaches
- Painful or swollen joints
- Fever
- Anemia (low numbers of red blood cells or hemoglobin, or low total blood volume)
- Swelling (edema) in feet, legs, hands, and/or around eyes
- Pain in chest on deep breathing (pleurisy)
- Butterfly-shaped rash across cheeks and nose
- Sun- or light-sensitivity (photosensitivity)
- Hair loss
- Abnormal blood clotting
- Fingers turning white and/or blue when cold (Raynaud’s phenomenon)
- Mouth or nose ulcers[4]
Along with these symptoms doctors can use a combination of blood and urine tests as well as physical examinations to determine if you have Lupus. While many tests can be used in the determination of your status, no one test can specifically diagnose Lupus at this time [2]. After dealing with fatigue Melissa's primary care doctor noticed a low white blood cell count and after a visit to a hematologist "the doctor kept an eye on my white [blood cell] count for about 4 more years, in which it fluctuated, until it took another dive. [Then] she sent me to a different hematologist, who jumped right on it, bless his heart." To confirm the possibility of Lupus Melissa underwent 3 tests (Anti DNA, C3/C4, and Epstein Bar) which determined her diagnosis. Over the coming years more symptoms surface. "I started experiencing bad joint pain, especially in my hands. It was bad enough that I had difficulty gripping anything."
Treatment and Living with Lupus

The drug regiment that may come be used to treat Lupus is highly dependent on personal symptoms and the doctors notes and expertise. Most often anti-inflammatory, antimalarial (drugs to treat malaria), corticosteroids (counter inflammation), and immunosuppressants (suppress immune system) are used[2]. For Mellisa her "joint pain is under control with Diclofenac, an anti-inflammatory, and [biggest struggle is] just managing [her] life and activity." Often times the best treatment for Lupus is just a healthy lifestyle and learning to manage the disease. Ensuring adequate rest, getting regular exercise, not smoking, and eating a healthy diet along with being sun smart can allow a patient to better cope with the symptoms they experience.
One of the hardest parts of living with Lupus is the uncertainty of when a flare up may occur and what it will be like when it happens. Marjorie explains an example, "Recently we were one hour in to a 3 hour drive when it hit out of the blue. We stopped at a gas station. 15 minutes later another stop. 15 minutes later another stop. We did this for about an hour until we got to a town where they have a CVS. I stayed at the CVS while my husband drove my son and his friend to their destination. I told the pharmacist what was going on in case it got worse and I needed to go to the ER for fluids. When my husband got me, a little over an hour later I had to stop one more time on the way home, and then I slept for 2.5 hours. I woke up when we got home, showered, and rested. The next day every part of my body hurt." From speaking with Melissa and Marjorie, there is no real trigger that seems to dictate when a flare is to occur. It is often a combination of lack of rest and stress / anxiety. Marjorie has done plenty of personal research on these flare ups, but still, "There has been no rhyme or reason with my attacks. I've done food journaling and that doesn't show anything. When I get overly fatigued I know I've just done way too much." More so, everyone with Lupus reacts and flares differently, meaning each individual will have to work to determine how best they can live with the disease[7]. Melissa says "The common symptom in all of us is fatigue, which makes day to day life difficult. When I'm having a flare, usually caused by not enough sleep or having a lot going on so I'm not able to budget my energy or rest, almost every joint in my body hurts. Even my toes and my jaw."
One of the hardest parts of living with Lupus is the uncertainty of when a flare up may occur and what it will be like when it happens. Marjorie explains an example, "Recently we were one hour in to a 3 hour drive when it hit out of the blue. We stopped at a gas station. 15 minutes later another stop. 15 minutes later another stop. We did this for about an hour until we got to a town where they have a CVS. I stayed at the CVS while my husband drove my son and his friend to their destination. I told the pharmacist what was going on in case it got worse and I needed to go to the ER for fluids. When my husband got me, a little over an hour later I had to stop one more time on the way home, and then I slept for 2.5 hours. I woke up when we got home, showered, and rested. The next day every part of my body hurt." From speaking with Melissa and Marjorie, there is no real trigger that seems to dictate when a flare is to occur. It is often a combination of lack of rest and stress / anxiety. Marjorie has done plenty of personal research on these flare ups, but still, "There has been no rhyme or reason with my attacks. I've done food journaling and that doesn't show anything. When I get overly fatigued I know I've just done way too much." More so, everyone with Lupus reacts and flares differently, meaning each individual will have to work to determine how best they can live with the disease[7]. Melissa says "The common symptom in all of us is fatigue, which makes day to day life difficult. When I'm having a flare, usually caused by not enough sleep or having a lot going on so I'm not able to budget my energy or rest, almost every joint in my body hurts. Even my toes and my jaw."
 The team stayed at Melissa's House during Redlands Cycling Classic
The team stayed at Melissa's House during Redlands Cycling Classic MaThere is no doubt that Lupus presents both physical and mental challenges. From visible effects of treatment, physical symptoms (pain, fatigue, etc.) to social ramifications such as physical limitations to work/activities, feeling social isolated, and managing within family and close relationships as they struggle to understand what you are going through[8]. People with Lupus can seem to be leading normal lives, but constant anxiety about the future, the next flare, and the progression of the disease constantly wear on patients. Melissa reminded me of this mental toll. "People need to be aware of just how difficult Lupus makes functioning on day to day basis, even to accomplish even routine tasks. They need to understand that the level of fatigue they feel when they have a cold is basically what we feel all the time because our immune system is constantly fighting. It never shuts off. Every day isn't horrible. I have good days too where I feel almost normal, but my definition of "normal" has changed over the years." Marjorie has similar feelings, "People will ask how I'm feeling, and I never say that I'm in pain or feeling tired or bad. I don't know what it is, but I just don't want people to know. I guess it's always polite to say you are doing well. But, if I'm asked to do something, and I'm not up to it, I do say no now. It's not worth it."
I hope to add more about the current state of research for the design, but for now I hope you would consider donating to the cause that would find a cure for the disease that affects, Mellisa, Marjorie, and 1.5 million other Americans. Thanks for reading!
Donate Here
Donate Here
References
- http://www.lupus.org/answers/entry/what-is-lupus
- http://www.mayoclinic.org/diseases-conditions/lupus/basics/definition/con-20019676
- http://www.webmd.com/lupus/guide/understanding-lupus-basics
- http://www.lupus.org/answers/entry/common-symptoms-of-lupus
- http://www.mollysfund.org/2013/01/diagnosing-lupus-and-lupus-tests/#1
- http://www.lupus.org/answers/entry/is-lupus-hereditary
- http://www.lupusresearchinstitute.org/lupus-facts/fight-lupus/living-with-lupus
- http://www.mollysfund.org/2013/02/coping-with-lupus-how-does-lupus-affect-your-state-of-mind-and-body/
Full Interview - Melissa
What was the diagnostic process like? How long did it take for the doctor’s determine you were suffering from Lupus
Initially, a low white blood cell count alerted my primary care doctor. At the time, a normal white count was between 4 and 10 thousand. Mine was 2.8. She sent me to a hematologist who said it was probably a virus that wasn't going away and to keep an eye on it. I was extremely disappointed, because I knew my excessive fatigue was more than just a virus and I wanted answers. My doctor kept an eye on my white [blood cell] count for about 4 more years, in which [time] it fluctuated, until it took another dive. She sent me to a different hematologist, who jumped right on it, bless his heart. He said before he did a bone marrow test, he wanted to send me to a rheumatologist to test for Lupus. At the time, I had no idea what Lupus was, and I was sure that's not with this was. I looked it up in the dictionary and the definition didn't describe what I was experiencing. I also was not having any other symptoms besides the fatigue and blood count. The rheumatologist ordered specific blood tests for lupus: Anti DNA, C3/C4, and Epstein Bar. I used to know what Anti DNA is, but I can't remember off the top of my head. If you want to know, I can look it up in The Lupus Book. It's a number that diagnoses lupus: above 50, you have lupus. Mine was 49. But along with the positive C3/C4, which is proteins in the blood used by the immune system, and the positive Epstein Bar, it was a positive diagnosis. After the diagnosis, I started experiencing bad joint pain, especially in my hands. It was bad enough that I had difficulty gripping anything.
What is the biggest challenge Lupus sufferer’s face
The challenges for Lupus sufferers are different from person to person, because it affects everyone in a different way. Each case seems to be specific to each individual. The common symptom in all of us is fatigue, which makes day to day life difficult. Those with severe cases have to deal with the effects of whatever is specific to their case. Personally, my joint pain is under control with Diclofenac, an anti-inflammatory, and just managing my life and activity. When I'm having a flare, usually caused by not enough sleep or having a lot going on so I'm not able to budget my energy or rest, almost every joint in my body hurts. Even my toes and my jaw. Another challenge is understanding by people who don't understand what it's like to live like this. To understand the level of fatigue on a day to day basis, and just because we look fine doesn't mean we are.
Can you describe what occurs during a “Flare Up” and what you do to manage it when it occurs
I think I kind of answered this in question 3. Basically, all the symptoms are just worse. For me, in addition to the joint pain, I have dry eyes and dry mouth, some degree of periphery nerve numbness in my legs (the surfaces of my lower legs and feet), and brain fog. And of course, the fatigue. So all of those are just worse during a flare (attack).
Is there anything else from your story of Lupus or from your experiences that people should know about these disease?
From my experience, people need to be aware of just how difficult Lupus makes functioning on day to day basis, even to accomplish even routine tasks. They need to understand that the level of fatigue they feel when they have a cold is basically what we feel all the time because our immune system is constantly fighting. It never shuts off. T cells tell the immune system to stop fighting and we don't have enough of them. B cells tell the immune system to start fighting and we have too many of them. So our immune systems are basically being given the order to fight an infection all the time and never given the order to stop, and when there's no infection to fight, it fights whatever it can latch on to.
Every day isn't horrible. I have good days too where I feel almost normal, but my definition of "normal" has changed over the years. But with every "normal" day I have, I still have to monitor my activity and make sure I overdo, because even though I may feel well enough to do more than usual, if I do too much, I'll pay for it for the next few days. So I may choose to do too much because, doggon it, there's things I want to do and accept that I'm gonna feel like crap. And then there's those inevitable emergencies in life that require me to step up and then I'm laid out for awhile.
In all this, though, Lupus has caused me to rely more heavily on my Lord for strength. There have been a few times that I should've been laid out because of one of those life emergencies, but I trusted Christ for strength and He was faithful. It has also given me tool to understand and empathize with people in similar situations, enabling me to encourage them, offer a shoulder and pray for them.
Full Interview - Marjorie
What was the diagnostic process like? How long did it take for the doctor’s determine you were suffering from Lupus?
I was seeing a dermatologist regularly and kept complaining about sores in my nose. It wasn't until at least a year later I went to my internist - who happened to also be head of Rheumatology at the hospital- for constant bruising on my legs, that some tests were done. This was 10 days before I turned 30. I had a two year old and was working 4 days a week and was totally exhausted. The ob/gyn would say something like: "you have a two year old; or a one year old; or you just gave birth. It's normal". Well I knew it wasn't. I had friends with children, and they weren't like me. When he told me, I had no idea what it was. I questioned why the dermatologist didn't realize it. I didn't take any medications for a long while. My ob/gyn at the time, did not take it seriously I didn't think. It was a disease like fibromyalgia and chronic fatigue that some doctors didn't think we're "real".
What is the biggest challenge to Lupus Research’s face today?
I think funding and that not everyone's symptoms are the same.
What is the biggest challenge Lupus sufferer’s face today?
Not knowing the cause, and not knowing exactly what will make one feel better.
Can you describe what occurs during a “Flare Up” and what you do to manage it when it occurs?
I can have extreme joint pain and extreme tiredness. When this happens I have to sleep. Another type of attack is stomach cramping. I never know immediately if this is going to be an attack or not. If it's an attack, I have to be near a bathroom, preferably also a place to sit or lie down. Recently we were one hour in to a 3 hour drive when it hit out of the blue. We stopped at a gas station. 15 minutes later another stop. 15 minutes later another stop. We did this for about an hour until we got to a town where they have a CVS. I stayed at the CVS while my husband drove my son and his friend to their destination. I told the pharmacist what was going on in case it got worse and I needed to go to the ER for fluids. When my husband got me, a little over an hour later I had to stop one more time on the way home, and then I slept for 2.5 hours. I woke up when we got home, showered, and rested. The next day every part of my body hurt.
Is there any clue as to what causes a “Flare Up” to begin?
No. There has been no rhyme or reason with my attacks. I've done food journaling and that doesn't show anything. When I get overly fatigued I know I've just done way too much.
Is there anything else from your story of Lupus or from your experiences that people should know about these disease?
People will ask how I'm feeling, and I never say that I'm in pain or feeling tired or bad. I don't know what it is, but I just don't want people to know. I guess it's always polite to say you are doing well. But, if I'm asked to do something, and I'm not up to it, I do say no now. It's not worth it.




























































 RSS Feed
RSS Feed
